Omada Health: A winning digital solution in chronic disease management
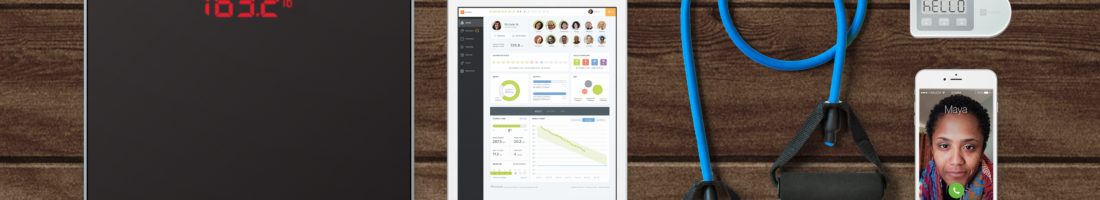
Omada’s digital behavioral health solution is a winning formula combining smart devices, personalized coaching, and innovative integration into existing healthcare structures to offer an outcomes-based model that improves health and lower costs.
In a healthcare environment that is facing increasing medical costs and an aging population wrestling with chronic illnesses, healthcare providers and businesses are shifting toward paradigms of technology-enabled value-based care, care coordination solutions, and customer-centric healthcare paid for by companies and insurance plans.
Omada Health (“Omada” or the “Company”) is one of the leaders in the digital behavioral health space. Omada offers technology-enabled disease management and behavioral counseling services to employers and health plans, targeting individuals concerned with obesity-related chronic diseases including type 2 diabetes, hypertension, and anxiety and depression. Led by CEO Sean Duffy, an HBS / HMS dropout who co-founded Omada in 2011, the Company has raised a total of $200 million in funding to date, with its most recent Series D funding round of $73 million (for a $600 million valuation) in June 2019 led by Wellington Management, alongside existing investors including Cigna, Sanofi, and Andreessen Horowitz. Other key prior investors include Humana Ventures and Kaiser Permanente Ventures.[1]
Personalized health for patients, comprehensive solution for employers
Omada creates value through a comprehensive integration of online and offline personalization to patients that creates behavioral change, as well as well-designed benefit management tools for employers. After identifying eligible participants from an employee base, Omada’s program pairs individuals with health coaches (from a pool of 130 coaches) who provide one-on-one support to patients.[2] They are guided by machine learning data that patients provide via wireless smart scales, blood pressure monitors, blood glucose meters, and a mobile app that tracks measurements including weight, physical activity, and food intake. Patients also have access to peer support groups (average 24 individuals per group) and interactive online lessons on nutrition, physical activity, and time and stress management.[3] These offerings encourage patients to engage and change daily lifestyle habits — a new model of treatment as compared to relatively infrequent doctors’ visits — which ultimately prevent the onset of diseases that later in life would become costly and impairing. Omada’s program is HIPAA-compliant and also includes systems that automate health insurance workflows like eligibility verification and claims submission, as well as marketing, data analysis and reporting to employers.
Innovative integration with existing healthcare structures
Omada is tackling areas of significant healthcare challenge and cost through a prudent expansion of its offerings into adjacencies that advance a care coordination model, while deeply integrating with regulators and businesses. Omada is the largest provider of the Diabetes Prevention Program (DPP) with over 85,000 users and is fully recognized by the Center for Disease Control and Prevention’s (CDC) as of May 2018.[4] After gaining traction in diabetes prevention, which was the Company’s initial product targeting a large addressable market of $237 billion, it soon moved into hypertension, mental health, and other chronic conditions. In January 2019, Omada entered into a perpetual licensing agreement for the software, curriculum and content of defunct startup Lantern, which provided CBT-based digital therapies to treat mental health conditions. Research has shown that obese patients are more likely to suffer from mental health issues such as anxiety and depression, which become a barrier to meeting physical health goals. While Omada historically screened patients for mental health conditions, it was unable to provide follow-up treatment and had to refer patients out to behavioral health specialists. The move into mental health was undertaken to address this care coordination challenge.[5] Meanwhile, Omada continues to seek further integration of smart devices into its diabetes type 2 offering, announcing in October 2019 a partnership with Abbott to integrate its FreeStyle Libre system, a continuous glucose monitoring (CGM) technology, into Omada.[6]
Success through outcomes
Omada’s outcomes-based revenue model is a key growth driver and differentiator that makes it competitive among cost-conscious employers and health plans moving toward values-based care. Employers, health plans and health systems pay the Company based on healthcare outcomes, such as patients’ weight loss or blood sugar level improvements. Omada claims that cost savings to an employer average $1,338 per participant by 24 months, and the program turns ROI positive at 6 – 12 months. The Company has built up the evidence base of its program by publishing 14 peer-reviewed clinical studies to date, which, among other results, show that Omada’s program results in average weight loss of 4.7% in a year and reduced risk of type 2 diabetes by 30%.[7] This intellectual property has enabled Omada to become a full medical provider, rather than simply a tech platform. Omada’s data shows that its outreach campaigns for participant enrollment are two times more effective than employer-led campaigns and participants engage with Omada on average 4.5 times per day.[8] To date, Omada has enrolled over 250,000 participants from over 600 companies (e.g., Cigna, Costco, Lowe’s) and including 35 health plans (e.g., Kaiser Permanente, Blue Cross Blue Shield Minnesota).[9]
Rapidly shifting industry dynamics
While Omada has had success signing on a number of private and state-level healthcare plans, there are still regulatory challenges ahead. Recently, the Center for Medicare and Medicaid Services (CMS) announced that they would not pay for digitally-administered diabetes prevention programs for Medicare patients.[9]
The digital behavioral health space has become crowded in recent years, and especially in diabetes prevention. In particular, rival Livongo, founded in 2008, has grown rapidly. Livongo offers a comparable product, claims to save $1,908 per participant per year in diabetes, and has signed on 208,000 participants and 771 companies (20% of the Fortune 500).[10] In April 2019, Livongo became the first consumer digital health company to partner with Amazon to allow members’ Alexa-enabled devices to read out blood glucose levels and health tips. In July 2019, Livongo raised $355 million through its initial public offering (stock down 10% to date, current market cap: $2.4bn).[11] Livongo and Omada have been competing head-to-head in coming to market with new offerings within weeks and months of each other (e.g., entry into mental health announced within weeks of each other in January 2019, introduction of cellular-connected blood pressure cuffs and glucose monitors within 7 months of each other, entry into hypertension within 6 months of each other).[12] Meanwhile other players abound in the digital diabetes and hypertension prevention and management space, such as Lark, Onduo (JV between Sanofi and Alphabet’s Verily), Virta Health, and Hello Heart.[13] To combat these pressures, Omada’s recent moves have shown agility in driving innovation in product breadth and depth and establishing partnerships across the healthcare system. To continue winning, Omada needs to keep up its execution of quality service, technology, and consumer engagement, and pursue more imaginative initiatives (e.g., cross-sector partnerships) that will drive further client uptake and ingrain its product in the everyday lives of patients.
References:
[1] https://www.cbinsights.com/research/health-insurance-corporates-investing-startups/
[4] https://www.omadahealth.com/press/press-release-omada-health-achieves-full-cdc-approval
[7] https://www.omadahealth.com/outcomes
[8] https://www.omadahealth.com/employers
[9] https://www.cnbc.com/2019/06/25/omada-health-raises-73-million-at-600-million-valuation.html
[10] https://ir.livongo.com/static-files/9158aba2-9d04-4a57-853e-f4b7ee0fb50e
[13] https://www.ft.com/content/0fee5b5c-a357-11e9-974c-ad1c6ab5efd1



This was a really informative post about a great example of a winner. I am glad you highlighted their success with outcomes, since relevant data is usually the biggest challenge in determining whether a digital health solution is a winner. I am very curious to see who wins in the Livongo/Omada battle. It may be more interesting if Omada also chooses to partner with a tech company like Apple or Google to increase their access to patients and expand their data set.