The Digital Solution to Overeating

Creating the "digital therapeutics" category
Can a digital solution have a greater clinical impact than a drug?
Problem & Solution
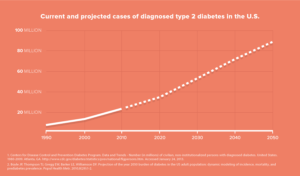
Chronic disease management sits at the bulls-eye of the healthcare cost challenge. Currently, chronic diseases account for “$1.1 trillion annually, or one-third of total US healthcare expenditures.”[i] Diabetes alone costs $230 billion.[ii] The disease affects 9.5% of the population and costs employers $4,500 per year in lost productivity and higher medical costs.[iii] Projected cases of diabetes are expected to skyrocket:
The most effective method of managing diabetes – even more so than powerful drugs like Metformin – is lifestyle changes, specifically avoiding a sedentary lifestyle and losing weight.[v] Realizing this, many physicians prescribe diabetes programs to help their patients lose weight. “The operating model of traditional diabetes programs involves a 16-week program at a brick-and-mortar, where the patient has to get in their car, drive to a center, sit there for 60-120 minutes, and potentially find a babysitter.”[vi]
Omada Health, a startup based in San Francisco, realized the friction in this operating model and developed a digital solution. The Omada Prevent program enrolls patients in groups of 10-12 into a 16-week program focused on healthy eating and exercise. Each group is assigned a “health coach”, who lends support through text messages and voice calls and tracks each patient’s progress digitally. The program is rooted in behavioral science and leverages the social networking power of groups; members encourage one another to continue to make healthy decisions. Prevent also features quizzes and learning modules; the digital operating model allows for asynchronous learning, as the material has been optimized for mobile, tablets, and laptops.[vii]
The Prevent program also provides patients with hardware, including a “zero-configuration” wireless scale and pedometer. The wireless scale and pedometer transmit weight and steps automatically to a private profile, shared only with the health coach. The scale also makes progress much more difficult to fake, a longtime problem in the space.
For those who successfully complete the program, the “Sustain” program offers lower touch follow ups to keep the weight off for the long-term.
Results
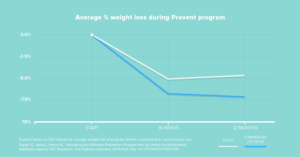
The combination of hardware, software, and behavioral science has produced impressive results:
In traditional in-person weight loss programs, typical engagement is in the 6-7% range and weight loss is roughly 2.4%. In comparison, Omada has shown engagement of 65% and weight loss of 4.7%. Not only that – Omada has published these results in third-party, peer-reviewed journals.[x]
Revenue model
Given the clinically-proven results and unorthodox solution, Omada sells the service with a revenue model more aligned with traditional weight loss programs. Omada uses a pay-for-performance billing model, where it does not collect fees unless it has demonstrated results. This is in stark contrast to typical diabetes weight loss programs, which charge for their service regardless of outcome. This revenue model has allowed Omada to scale to over 20,000 participants as of 2015 with blue-chip customers such as Kaiser, Humana, Lowe’s, Iron Mountain, and Costco.[xi]
Omada is also well-positioned for several developments in the healthcare landscape:
- Shift in reimbursement model to fee-for-value. The US healthcare system is transitioning from fee-for-volume to fee-for-value, where provider reimbursement levels are tied to quality outcomes. Omada is well positioned for this shift as its solution is both scalable with low incremental costs and twice as effective as current treatment.[xii]
- Increased burden for consumers to pay for care. Many employers have adopted coverage shifting cost burden onto employees in the form of higher premiums, deductibles, and cost-share. As consumers become less insulated from large bills, they have become more willing to adopt cost-effective digital tools to manage their health, including Omada.[xiii]
What’s next?
Omada has created a new category of digital therapeutics and can take a number of steps to improve its offering. First, Omada can push healthier behavior in more high-touch (and potentially intrusive) ways. Omada could consider giving its patients weights with sensors to monitor how much they exercise. Perhaps the company could also push notifications to its users when they are making food choices e.g. at the grocery store or in their home pantry. Omada could also consider moving “upstream” to remote tracking devices related to diabetes – perhaps integrating with IoT glucose monitors or blood pressure monitors to create a fuller view of diabetes management for a clinician. Lastly, Omada should consider expanding to more chronic disease states. The coaching plus technology approach can encourage better behavior for those looking to quit smoking, beat insomnia, and control hypertension.
Word Count: 735
—–
[i] David Roman and Kyle Conlee, “The Digital Revolution Comes to US Healthcare”, Goldman Sachs, June 29, 2015.
[ii] Ibid.
[iii] Alexander Fogel and Joseph Kvedar, “Simple Digital Technologies Can Reduce Health Care Costs”, Harvard Business Review, November 14, 2016, https://hbr.org/2016/11/simple-digital-technologies-can-reduce-health-care-costs?utm_source=feedburner&utm_medium=feed&utm_campaign=Feed%3A+harvardbusiness+(HBR.org), accessed November 2016.
[iv] Balaji Srinivasan, “Software Gets the World to Stop (Over) Eating”, Software is Eating the World (blog), Andreesen Horowitz, April 9, 2014, http://a16z.com/2014/04/09/omada-health-behavior-change/, accessed November 2016.
[v] Diabetes Prevention Program Research Group. “Reduction in the Incidence of Type 2 Diabetes with Lifestyle Intervention or Metformin.” New England Journal of Medicine. Volume 346, Number 6. February 7, 2002. p. 393-403.
[vi] Arundhati Parmar, “Why Intermountain chose Omada Health to provide diabetes prevention services”, MedCityNews, August 2, 2016, http://medcitynews.com/2016/08/intermountain-chose-omada-health-provide-diabetes-prevention-services-patients/, accessed November 2016.
[vii] Omada Health. “About Us.” https://www.omadahealth.com/about, accessed November 2016.
[viii] Omada Health. “Our Solution.” https://www.omadahealth.com/solution, accessed November 2016.
[ix] Balaji Srinivasan, “Software Gets the World to Stop (Over) Eating”, Software is Eating the World (blog), Andreesen Horowitz, April 9, 2014, http://a16z.com/2014/04/09/omada-health-behavior-change/, accessed November 2016.
[x] S. Cameron Sepah, Louhua Jiang, and Anne Peters. “
Translating the Diabetes Prevention Program into an Online Social Network.” The Diabetes Educator. Vol 40, Number 4. July/August 2014. p. 435-443.
[xi] Omada Health, “Omada Health Raises $48 Million to Fight Obesity-Related Chronic Disease,” September 16, 2015, https://www.omadahealth.com/news/omada-health-raises-usd48-million-to-fight-obesity-related-chronic-disease, accessed November 2016.
[xii] David Roman and Kyle Conlee, “The Digital Revolution Comes to US Healthcare”, Goldman Sachs, June 29, 2015.
[xiii] Ibid.



Great post. This is really interesting. I wonder if Omada should considering expanding as a fitness program for people without diabetes or other chronic diseases. To bring down healthcare costs, we really need to somehow prevent people from getting chronic diseases in the first place where avoidable. As we learned in StickK, the social aspect of these programs actually do help people achieve their goals. Personally, I use a workout plan in which a trainer I see only once a month can track my workouts and make adjustments remotely. Because we are also friends, I feel extremely guilty if I miss a workout, and it has been very effective to keep me on track, much more so than some monetary reward would be, or even a desire to be fit. I know Omada already uses the community but I wonder how involved they get non-diabetic family and friends, which could be quite effective.
Interesting post and company! The “pay for performance” revenue model reminds me a of the Stikk case we did in marketing, however I think that Omada has a better model because it partners directly with Kaiser, Humana etc. In the Omada model the company pays for performance instead of the individual. I would imagine if the individual had to pay for performance, the accuracy of reporting would decline so they did not have to pay fees.
Another next step to elevate Omada’s value prop is to have a diet component / food component. Companies such as Rise (https://www.rise.us/#) offer apps where you can text a dietitian everything you eat and the dietitian will respond and offer advice / encouragement. This keeps users accountable to a real person with the food they eat.
Thanks for sharing this – I hadn’t heard of Omada before and it sounds like a compelling business in the healthcare space! As the other comments mentioned above, I really like the distinctive pay-for-performance model billing model that is covered by Kaiser, Humana, etc. This would would ensure that people’s reporting is more accurate and not skewed to avoid paying the fees.
Overall, I think this integrated hardware / software approach is novel and innovative for tackling diabetes / heart disease programs, particularly when the current operating models are burdensome and lack social support. I do however have a few concerns that may inhibit customer acquisition. First, I wonder if certain customers who have the peer groups would feel peer pressured in a negative way by seeing others performance or having notifications of others doing activity while they are not. This could induce additional stress that may in fact increase health concerns related to diabetes. Second, I also am curious to know how the messaging with the health advisor works — it could be best to have it controlled to certain time frames so the user is not over burdened.
I really liked this model and this there are avenues for further growth. The company could easily partner with fitness organizations to have trainers for user and / or Nike to utilize some of their fitness programs that they have on their fitness app. Additionally, they can partner with retailers of organic / health foods / vitamins to make these available at discount for users so that they can purchase their meals from there.