Iora Health: Getting People to Pay for Prevention
Iora Health uses a unique operating model to improve health outcomes in primary care.
Iora Health was started in 2011 with the aim of reducing health care costs by getting people to use more primary care. Founder Rushika Fernandopulle started the company with the intent to make patients healthier at lower cost by increasing access to primary health care services. Originally a small primary care practice in Arlington, MA, the company now has 14 sites, each consisting of one to three clinics that partner with a local employer, insurance plan or union to provide primary care to all enrolled employees. The company has a well designed operating model that supports its business model.

Iora’s business model rests on the principle that investing in primary care now will save money in ER visits and hospitalizations in the long run. This model requires that people spend more, not less, money on primary care services, with the expectation of savings in the future. It also requires that providers are incentivized to focus on quality of care rather than volume. Neither of these concepts are revolutionary, but Iora has a unique operating model that effectively aligns processes and incentives to actually achieve its stated aims. There are 3 key factors underlying the successful alignment of the business and operating models at Iora:
1. Financial incentives
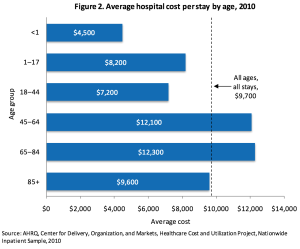
Iora’s payment system incentivizes quality of care over volume. The company charges employers a flat monthly fee of about $50-60 per month for all of the employees enrolled in their plan. This fee is actually double what companies typically pay for primary care but necessary in order for Iora to provide the more in depth services that form their core business. The company justifies the expense because it pails in comparison to a single hospital stay, an outcome Iora aims to avoid. Iora justifies this pricing through its philosophy that investing in primary care now keeps patients out of the hospital and saves on big bills later. Doctors are paid a fixed salary rather than being reimbursed on a fee-for-service system, which would push them to see as many patients are possible in a given amount of time to maximize profit. As such, a one-hour visit would be unheard of in the standard primary care setting. At Iora, care providers are actually encouraged to treat a patient effectively and set up a good system of follow up. The more the patient is empowered to help themselves on a daily basis, the fewer visits they will need and the lower Iora’s costs become.
2. Labor utilization
Labor costs are contained by employing health coaches, nutritionists and personal trainers who follow up with patients and help them adhere to their health goals. This improves patient compliance with the physician’s plan without tying up the physician’s time. The health coaches, whose previous jobs range from cashiers to customer service agents are well trained for their specific jobs, but command a much lower salary than the doctors or nurse practitioners. For patients with mental health issues, there’s a behavioral health specialist on staff, again not a doctor, to go through initial questions. In mental health, successful therapy relies as much on the conversation as it does on medication so this again allows Iora to provide high quality care at a lower cost than a psychiatry clinic. All of these services are in line with the payment structure, which rewards employees when patients don’t need to return. The coaching staff can help patients take care of social and lifestyle factors, which are significant drivers of health outcomes, so that the doctors’ time remains free for the most complicated cases.
3. Immediate feedback
Electronic health records are well integrated into patient care and used both to collect information and actively manage patients during and after visits. The system can track patients’ key goals and alert coaches and providers to any possible issues as soon as they arise. For example, the clinic is notified if patient fails to pick up a prescription and a health coach is on hand to reach out for assistance immediately. This investment in early detection of compliance issues reinforces the core principle of the business model, that fixing issues now will save healthcare dollars later. Helping a patient getting their medications immediately prevents serious conditions like chronic obstructive pulmonary disease (COPD) or congestive heart failure from going untreated and leading to dangerous and costly hospitalizations. Patients also have access to their own records to allow open communication between providers and patients and make patients feel more in control of their care.

The major remaining obstacle to Iora’s success is that the business model itself hasn’t yet been proven. With only 4 years of data, there isn’t clear, convincing evidence yet that this investment in primary care will pay off with sustained lower hospital bills in the long run. Early numbers from Iora’s first clinic in Atlantic City, NJ suggest that enrolled patients did have fewer ER visits and hospitalizations than the control population and that their overall health care costs were 12.3% lower. Multiple clinics have seen small victories in cost containment, such as an increase in generic prescription rates. However, whether or not this model can scale to include a more diverse group of patients remains to be seen. At the end of the day, prevention is a difficult thing to sell as people tend not to value their health until its gone. Nonetheless, from an operating perspective, Iora is well positioned to succeed, should their core hypothesis prove true.
Sources:
Iora Health
http://www.iorahealth.com/
http://www.newyorker.com/magazine/2011/01/24/the-hot-spotters
http://www.ihi.org/education/ihiopenschool/blogs/_layouts/ihi/community/blog/itemview.aspx?List=9f16d15b-5aab-4613-a17a-076c64a9e912&ID=95
http://www.bizjournals.com/boston/blog/startups/2012/08/iora-health-boston-primary-care.html?page=all
http://www.nationaljournal.com/next-america/newsdesk/radical-rethinking-primary-care-that-could-make-everyone-healthier



Thanks for this post, Gaurie. Great to see some innovative solutions being experimented with to help the overburdened healthcare system. I would be curious to get your thoughts on how sustainable you think this business model is. In particular, are doctors likely to make enough money earning a fixed salary to ensure they do not switch to clinics with a more traditional business model? And, how many years of data are employers going to need to see to be convinced to pay higher premiums up front?
Gaurie – really interesting post and neat way to execute a network that takes advantage of the benefits of preventative health. There are many challenges to this as you’ve highlighted, but what I’m worried about is that the benefits of preventative care are created over the long term (ie spending extra on health for employees in their 20s-30s so you spend less in their 50s-60s). Given that employee tenure at companies is so low, it seems as though employees will need to bare the burden of the increased costs. How can they incentivize people to pay more for healthcare than they need to? The benefits of preventative care are well known, yet people dont do it today.