Hanging Gardens of Healthcare or Tower of Babel?

A young U.K. startup by the name of Babylon Health is capitalizing on the existing capacity of mobile phones as a medium to connect patients with general practitioners. Their mission is to put “accessible and affordable health service in the hands of every person on earth.”
The healthcare industry is ripe for digital disruption. A young U.K. startup by the name of Babylon Health is capitalizing on the existing capacity of mobile phones as a medium to connect patients with general practitioners. In fact, they have created an integrated digital health service which they aim to put “in the hands of every person on earth[i].”
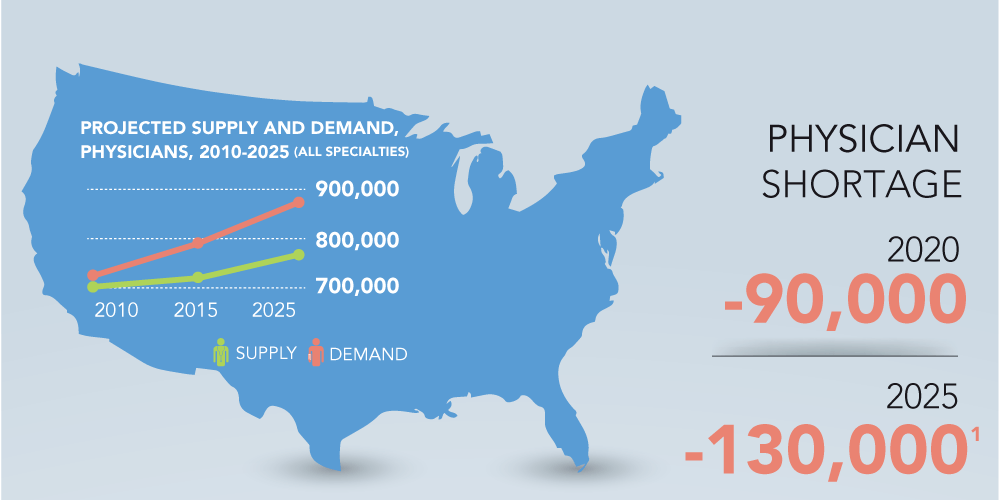
The World Health Organization estimates a current global shortage of 7.2 million health care workers, a number it expects to double by 2035. Babylon Health believes that diagnosis through technology can scale much more rapidly than the production of doctors[ii]. Founder Ali Parsa argues that the preponderance of our healthcare needs has little to do with hospitals, but rather simple diagnostics or consultations. Yet we schedule appointments weeks in advance, take half the workday off, and wait hours to be seen[iii]. Babylon Health is attacking this inefficiency.
Source: Bartonassociates.com
The company provides a subscription service through its smartphone app, which uses an A.I. chatbot to query and triage patients for a practitioner. The patient can then consult virtually on demand with a general practitioner (GP) through their phone. GPs diagnose and prescribe medication for delivery to the patient or advise an in-person visit if necessary[iv]. Says Parsa, “I’d trust a machine over a human any day of the week – and I already do…[e]ven highly-trained and competent medical professionals are not infallible[v].” The company claims 92% accuracy in its diagnoses, while doctors and nurses are 82% and 77% accurate respectively. Currently, the average doctor performs 7,000 consultations each year. Such technology could dramatically improve overall capacity by decreasing patient traffic at hospitals, increasing speed and accuracy, and increasing patient throughput per doctor. The A.I. will never replace doctors, but in the next 10 plus years it can be a more precise compliment while costing 80% less per hour to treat a patient[vi].
Critics are concerned that firms like Babylon Health are cherry-picking talented GPs away from an already dwindling pool. Competitors like HealthTap employ 60,000 doctors, which are paid per consultation. Babylon, however, employs a full-time cadre of 100 doctors, which minimizes the siphoning of existing GP pools, minimizes costs, and allows Babylon to offer cheaper prices than competitors[vii]. Others are wary that mobile treatment risks fragmenting health services to the public by attracting younger, healthier people while excluding those with chronic and mental illnesses, pregnant women, and elderly which require specialists. While it is difficult to predict if this technology will further stretch or fragment the GP population, much depends on the integration and adoption of existing organizations. Babylon does not intend to compete with the U.K.’s publicly funded National Health Service (NHS). Rather, the technology is backed by the NHS, which has now reduced wait times to minutes[viii]. Such alignments should also serve to create synergies in allocation of GPs and reassessing hospital patient demographics.
Babylon has tested a variation of its concept in Rwanda for the past year. The shortage of doctors and queues at clinics are no different, but austere environments and poor populations add a new twist. Babylon set up kiosks around the country and now provides services to over 600,000 Rwandans for less than a dollar per consultation[ix].
As Babylon Health expands and experiments, it will certainly need to modify its technology in developing nations to achieve its end state. Until mobile phone and internet can further penetrate developing markets, Babylon may have to modify its delivery mechanisms. Most importantly, the company must transparently synchronize efforts with government and private health organizations to ensure a lasting solution. Moving forward, should Babylon apply the “kiosk method” to reach other emerging nations before internet and mobile networks do? Could this work in the current U.S. healthcare environment?
[783]
[i] Babylon Health, “The Babylon Purpose, https://www.babylonhealth.com/our-mission/, accessed November 2011.
[ii] Loder, Natasha, “Is There a Doctor in My Pocket?” The Economist: 1843, (October/November 2017): https://www.1843magazine.com/technology/is-there-a-doctor-in-my-pocket, accessed November 2017.
[iii] Solon, Olivia, “Babylon app puts a GP in your pocket,” Wired, (28 April 2014): http://www.wired.co.uk/article/babylon-ali-parsa, accessed November 2017.
[iv] Rogers, Charlotte, “Meet the healthcare disruptors treating patients like demanding consumers,” Marketing Week (Online), (8 June 2017): ABI/INFORM via ProQuest, accessed November 2017.
[v] “Revolutionising healthcare: What part does tech and industrial design play?” medGadget, (2 October 2017): https://www.medgadget.com/2017/10/revolutionising-healthcare-part-tech-industrial-design-play.html, accessed November 2017.
[vi] Murgia, Madhumita, “How smartphones are transforming healthcare,” Financial Times, (12 January 2017): ABI/INFORM via ProQuest, accessed November 2017.
[vii] Olson, Parmy, “The A.I. Will See You Now,” Forbes, 22, (12 November 2015): Business Source Complete, EBSCO, accessed November 2017.
[viii] “Why doctors are worried about an NHS smartphone app offering 24-hour GP consultations,” Sunderland Echo, (6 November 2017): http://www.sunderlandecho.com/news/health/why-doctors-are-worried-about-an-nhs-smartphone-app-offering-24-hour-gp-consultations-1-8843071, accessed November 2017.
[ix] “Doing More With Less,” Health Care, The Economist, (11 November 2017).



I agree with both angles you took on this, one being the obvious that digitizing healthcare will reduce costs and demand for doctors. But I appreciated the more unique viewpoint of looking at it from a lens of patient convenience and accuracy. I imagine this accuracy comes a lot from cutting down on stresses that many medical establishments currently face and allowing doctors to diagnose in a more relaxed environment with access to more resources than they would have in a hospital environment while speaking to the patient. I think digitizing medicine scares a lot of people because they worry that it is a step towards eliminating any human interaction in medicine. But like you said I think there will always be a need for medical professionals and patient – doctor interaction, but transferring the simple things to a computer will allow doctors to do their jobs better by eliminating some of their workload.
I think that there is certainly potential for telemedicine providers like Babylon to improve access to healthcare for certain populations, particularly in low-resource setting like Rwanda where there is a significant shortage of physicians and many patients may have no other options. These models also generally work best for one-off, high urgency but low acuity issues like sinus / ear / urinary tract infections or prescription refills, with more complex issues requiring an in-person visit.
We actually looked at a similar company when I worked in healthcare VC, and we ultimately decided not to invest. One of the primary reasons was that the utilization/adoption data for companies like this has actually been pretty poor. This was very surprising to me because I thought that these solutions offer a significant convenience advantage for the reasons you outlined above. But it seems that for the most part, patients are unwilling to forego traditional face-to-face visits with a healthcare provider, even when inconvenient. Perhaps this will change over time, but it has taken much longer to see adoption than many in the industry expected. Another reason we were bearish is that these models don’t work in favor of entrenched healthcare players that are reimbursed per visit, as you mentioned above.
That said, in the long run I am very optimistic about the ability for AI and other emerging technologies like Babylon to improve care and increase capacity. Theoretically as the healthcare system moves toward more value-based arrangements the economic barriers should fall away. I would also assume that people will become more comfortable with receiving care via call, text, or video as time goes on. I just hope we can get there sooner rather than later!
Thank you for raising this topic – while reading this article, I am asking myself why does this technology and platform not already exist on a large scale and why isn’t this how we run the healthcare system? I think the answer is a LEAD one. The customer promise of having access to a doctor is an important one, but if you can get convenience, speed, accuracy, and cost – then perhaps consumers can bypass an actual exam. However, the doctors may not want this. This commoditizes their specialty and they will want to protect that as much as possible. Also, the health regulatory environment is also set-up to be complicated and have a lot of moving pieces so that each piece can make money in the process. This would make the health care system smoother but also take out cost (and thereby value for many players).
The consumers have the most to gain from this and companies such as this should be pushing forward their agenda full on!